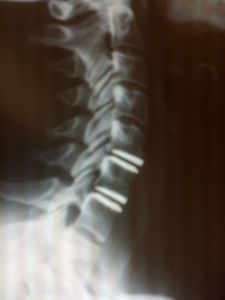
Cervical Disc Replacement
What are Cervical Disc Replacement benefits?
Cervical disc replacement surgery allows to free patient from neck pain and radicular pain (arms / hand).
- >90% Success Rate

- Early postoperative neck motion
- Preserved normal neck motion
- Reduced degeneration of adjacent sections of the cervical spine
- Exclusion of the need for a bone graft
- Quicker return to normal activity
- No bone grafting is required
- There is no need to install a plate for stability
- Motion of the spine is maintained, which may protect adjacent levels from wearing out
- Less chance of second surgery (re-intervention) in comparison with ACDF
Who is a candidate for Cervical Disc Replacement?
Any person without contraindication and substantial neck and/or radicular pain (arms, hands).
Cervical Disc Replacement Contraindications
• Cervical Trauma
• Cervical Ossification
• Long term degenerative changes
• Osteoporosis
• Significant facet joint pain component
What is Cervical Artificial Disc Replacement?
Cervical artificial disc replacement is used to treat symptomatic cervical disc disease that has not responded to nonsurgical treatment and is impacting upon the patient’s quality of life and ability to function normally. It is also known as total disc arthroplasty.
Cervical discs are the cushions or shock absorbers between the bones (vertebra) of the cervical spine (neck). Discs that are damaged either through injury or degeneration, such as disc herniations, can cause pain, numbness and weakness. When a disc moves out of its normal positions and becomes compressed, frayed, and/or herniates into the adjacent spinal canal it can put pressure on the individual nerve roots that exit from the spinal canal at each vertebral level or on the central spinal cord. This can cause the body to produce spurs called osteophytes which form over a period of time and can also cause pressure on the spinal cord or nerve roots, resulting in pain.
Cervical disc replacement is a surgical procedure to replace a damaged or degenerated cervical disc which has been surgically removed in order to relieve compression on the spinal cord or a nerve root, which is a source of pain for the patient. An artificial cervical disc device is used as the replacement, which is inserted between two cervical vertebrae. It is an alternative to the traditional and more common anterior cervical discectomy and cervical fusion surgery where the affected disc is replaced with bone grafts from the patient or a human cadaver or cervical cages (made out of PEEK or Titanium), and plates and screws.
The purpose of the artificial disc device is to preserve motion at the disc space and to reduce or eliminate pain for the patient.
Cervical artificial disc replacement is a newer and technically challenging procedure whose exact indications continue to evolve, and more data from clinical trials is released yearly where safety and effectiveness results are analyzed. Clinical results from FDA trials in the United States found that they were equivalent (if not slightly superior) to the traditional methods of anterior cervical discectomy and fusion.
It is important to note that cervical disc replacement is now an FDA approved option for surgically treating symptomatic cervical disc disease but has only been available in the United States in recent years, and it is only approved for use at one cervical level and is not approved for use adjacent to a previous cervical fusion. In Europe it has been available since the 1990’s and can be used at numerous cervical levels.
In the majority of cases cervical artificial disc replacement surgery can be performed however there are certain circumstances in which it is not an option, for example, if the patient has an active infection or significant osteoporosis; when there is abnormal motion or instability at the affected level; when there is advanced degenerative changes known as spondylosis affecting the facet joints in the back of the spine at the affected level; and in children.
Patients need to discuss whether disc replacement is an option for their specific condition with a qualified spine surgeon.
 How does it work?
How does it work?
Surgery is performed with the patient under general anesthesia and positioned face up. A one to two inch (3-5cm) horizontal incision is made on one side of the patient’s neck (usually right side) and the affected disc is removed from between the two vertebrae and the space is carefully filled with a disc replacement device and the wound is closed. A microscope or surgical magnifying glasses are usually used to aid the complete removal of the disc and live x-ray called fluoroscopy can be used to allow proper positioning of the implant.
The disc replacement device is typically made using two metal implants, though some devices use other materials (PEEK or plastic). One surface is attached to the upper vertebra and the other to the lower vertebra. These surfaces are either able slide directly on each other or can be separated by a piece of medical grade plastic, permitting motion between the two vertebrae to be maintained. The device can be held in place with screws or sometimes by a press fit anchor that secures the implant to the bones.
Patients are normally able to be discharged from hospital on the same day or the following morning post-surgery. The use of a cervical collar normally it’s not necessary. Post surgery pain is usually limited and improves significantly within two to three days. The nerve symptoms such as pain, numbness, and weakness that were being treated are often dramatically improved within hours of the surgery (however in some cases it can take weeks or even months to recover). Following surgery, X-rays are taken to confirm the proper positioning and functioning of the disc replacement device. Most patients are able to return to light work after a week or two post-surgery and resume normal life six weeks afterwards.
Exclusion Criteria for Cervical Artificial Disc Replacement
- Marked Spondylosis/Facet Joint Arthrosis
- <2º motion at index segment
- >50% disc space collapse
- Segmental Instability (>3 mm translation)
- Cervical Kyphosis
Sources:
Dr. Vicenç Gilete, MD, Neurosurgeon & Spine Surgeon.
Neurosurgery volumes I–III. Edited by Robert H. Wilkins and Setti S. Rengachary. McGraw-Hill.
Handbook of Neurosurgery. Mark S.Greenberg, Seventh Edition. Thieme.
Last Update [site_last_modified date_format=”Y-m-d H:i:s”]
info@cervicalspinespecialistcenter.com